A 20-year journey of health research in BC: Bringing hope and healing through emerging therapies
30 August 2021

Dr. Shannon Dames
Dr. Shannon Dames: Bringing hope and healing through emerging therapies
Dr. Shannon Dames teared up as she recalled sending a mass email to her colleagues at Vancouver Island University (VIU) with the subject line: “WE WON!” It was 2018, and she had just been notified that she had received a treasured MSFHR funding award for her research in mental health and resiliency.
As a small institution with faculty members teaching full time, the excitement that ensued from the team was incredible. “Our little part of the world was celebrating,” says Shannon. She describes being on her last legs before receiving the funding award, burning the candle at both ends, often late into the evenings and on the weekends to balance her research, a full teaching schedule and a young family. The award was a significant achievement, giving her the confidence to continue down the path of research and providing much needed financial support for her and the team at VIU.
“As caregivers, therapists, doctors, you are assumed to come into this work as fully resourced individuals, and that simply isn’t the case. I feel like I tried every single door and none of them worked, so I became a researcher to find a door for myself, where there wasn’t any in the system.”
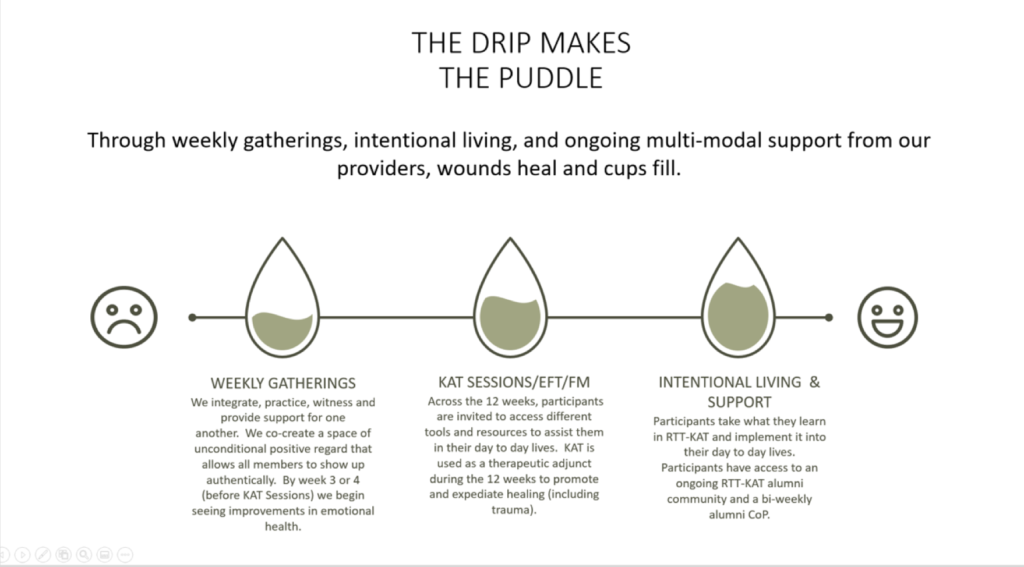
Supported by the MSFHR 2018 Reach Award, Shannon and her team developed the Roots to Thrive (RTT) program, an evidence-based curriculum that enables caregivers facing burnout to succeed and flourish in high-stress situations. The powerful program is based on a community of practice model, which encourages caregivers with shared concerns and passions to come together to support individual and collective healing.
Shannon’s initial curiosity that led to her research came from her personal experiences as a young adult being pushed out of her home, and her experience as a caregiver in high-stress environments. As a frontline nurse, Shannon and many of her colleagues encountered burnout and mental health exhaustion. She found herself trying to deal with her own trauma while managing the care of her patients. “As caregivers, therapists, doctors, you are assumed to come into this work as fully resourced individuals, and that simply isn’t the case. I feel like I tried every single door and none of them worked, so I became a researcher to find a door for myself, where there wasn’t any in the system.”
Although frustrating, this experience led her to understand the power of a community-based healing model, which she placed at the heart of the RTT program. “I learned that we do not heal alone. It’s working in community, in groups and in relationships where we start to see some of the condensed healing and shifts happen.” In the years since the program launched, Shannon has reported improved resilience, mental wellness and cognition in participants. She has also gone through the program and attributes its learnings to her own healing journey.
“For a long time, funding seemed unreachable. Michael Smith Foundation breathed life into our institution.”

In 2020, Shannon and her team were once again successful in their application for MSFHR funding, receiving a Health Professional-Investigator award co-funded by MSFHR in partnership with the Lotte & John Hecht Memorial Foundation. The partnered award is allowing her to build upon the success of the RTT framework by combining the program with emerging psychedelic therapies. The team use dosing ranges that optimize the psychedelic (mind manifesting) effects of ketamine. Ketamine, historically used by doctors as an anesthetic, is now gaining attention as a therapy for mental health. By studying and reporting on the process including learnings, facilitators and barriers, Shannon’s research will provide a roadmap for how psychedelic-assisted therapies can be used in Canada. This research process is complicated by current policy challenges. “Ketamine is currently the only legal avenue for [patients] to experience psychedelic-assisted therapy unless they go into the underground [market],” she explains. “For this reason, we are starting with ketamine, which will enable us to develop the infrastructure necessary to support the other psychedelic medicines when they become available. As part of this development, the next step for this first RTT-KAT trial is to provide therapists with experiential training that is safe and legal.”
Shannon hopes to expand the RTT framework to include additional psychedelics and patient groups, bringing hope to many like herself who are looking for support. She is grateful to MSFHR for recognizing the smaller institutions and the potential in her research. “For a long time, funding seemed unreachable. Michael Smith Foundation breathed life into our institution.”
Despite the long hours and constant hustle of being a researcher, Shannon is motivated by the personal applicability of her research, as well as the hope it brings. “I have a lot of juice and drive to find out what factors can impact my own and other’s healing. It’s exhilarating to watch others heal, especially those who believe they are truly unhealable. When you watch these emerging therapies help people unfold and bloom in the world, it provides hope.”
Learn more:
Roots to Thrive (RTT) and RTT-KAT
Combining Psychedelics with Therapy to Manage Mental Health (MSFHR, May 2021)
Dr. Shannon Dames Encourages Others to Find their “Roots to Thrive” (MSFHR, November 2019)